Mike Piskie
Mike Piskie
This UAB tertiary teaching-hospital study found that patients who developed hospital-acquired pressure ulcers incurred substantially higher costs and longer stays. Adjusted analyses showed costs of $29,048 vs $13,819 and length of stay of 20.9 vs 12.7 days, confirming pressure ulcers independently drive excess inpatient utilization beyond baseline severity.
This UAB tertiary teaching-hospital study found that patients who developed hospital-acquired pressure ulcers incurred substantially higher costs and longer stays. Adjusted analyses showed costs of $29,048 vs $13,819 and length of stay of 20.9 vs 12.7 days, confirming pressure ulcers independently drive excess inpatient utilization beyond baseline severity.
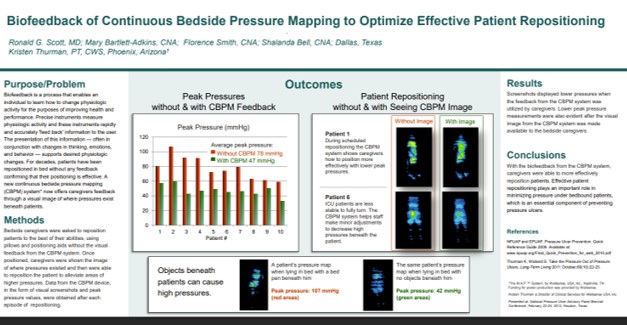
At a Dallas-area long-term acute care facility, real-time pressure visualization reduced average peak pressures by 40% – from 78 mmHg to 47 mmHg. 100% of caregivers reported more effective repositioning with the pressure image than without it, including for patients too medically complex to fully turn. Hidden objects beneath patients – including a bedpan producing a peak pressure of 107 mmHg – were identified and resolved immediately through visual confirmation.