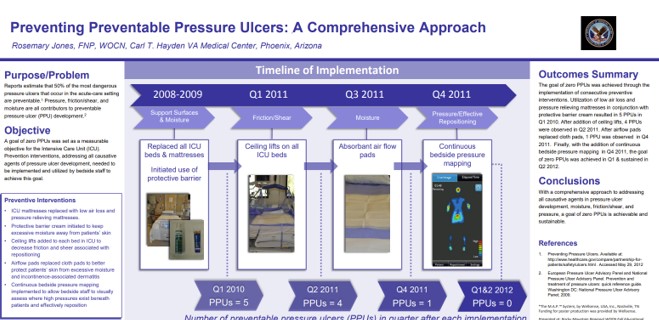
This real-world clinical poster from Floyd Medical Center shows that using a real-time pressure visualization monitor led to a 71% reduction in hospital-acquired pressure injuries (HAPIs) over 5 months in the critical care unit, by guiding staff to reposition patients more effectively and reduce peak pressure exposures.
 Mike Piskie
Mike Piskie
When appropriate patients were identified as able to self-turn, real-time pressure visualization helped them reposition themselves reliably with clear, immediate feedback. This demonstrates that pressure visualization can actively engage patients in their own pressure management, supporting safer self-directed turning when clinically appropriate.
In two UK NHS hospitals, continuous bedside pressure mapping helped identify and reduce pressure ulcer incidence, with staff reporting 100% agreement that the system improved positioning, reduced risk, and was beneficial in care. Patients and families also responded positively, with 78% rating the system helpful.
In a veteran population, pressure visualization was used not only to guide clinical care but to empower patients and caregivers with understandable, visual information about pressure risk. This supports greater patient involvement in day-to-day positioning decisions and reinforces shared accountability for prevention and healing.
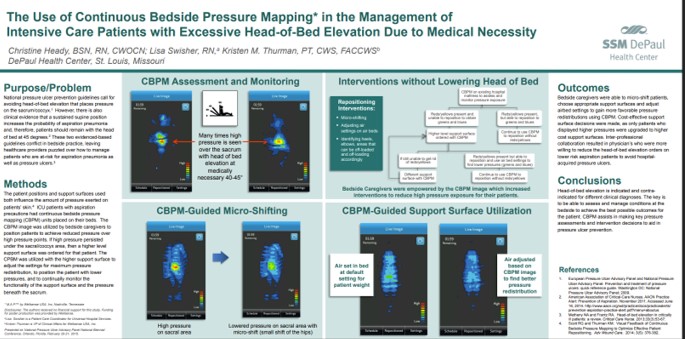
SSM DePaul Health Center showed that continuous bedside pressure mapping identified dangerously high sacral pressures at 40–45° head-of-bed elevation, enabled simple micro-shifts to reduce pressure, and guided use of higher support surfaces only when truly needed—improving outcomes and lowering costs