Real-Time Pressure Assessment and Monitoring With a Fluid Immersion Simulation Support Surface Show Clinical and Financial Benefits for Flap Management
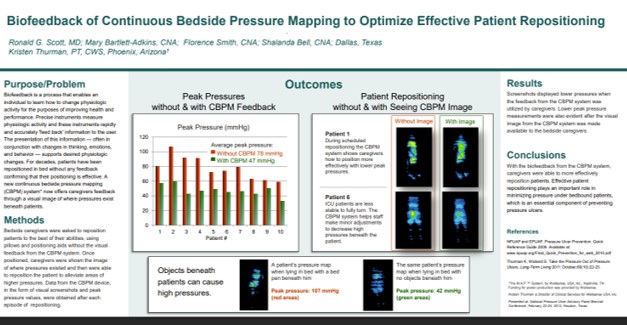
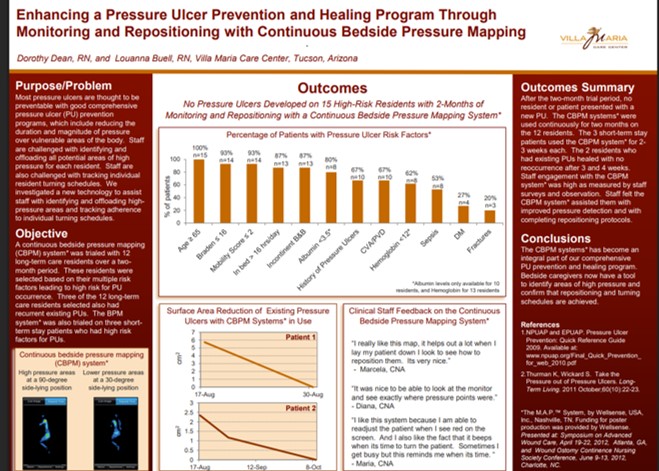
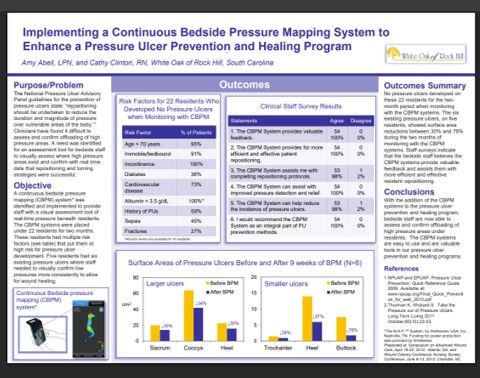
Visual feedback from continuous bedside pressure mapping enabled caregivers to reposition patients more effectively, lowering high pressures and improving care