Select a category to explore
Title
High cost of stage IV pressure ulcers
Key Takeaway/s
This study from NYU School of Medicine found Stage IV pressure ulcers cost about $125k–$129k per patient in hospital treatment costs when ulcer-related complications were included. These costs are far higher than prior estimates and emphasize early recognition and treatment to stop progression to Stage IV and avoid extreme, non-reimbursed “never event” costs. Read Full Article
Title
Key Takeaway/s
Analyzing 1.25 million US patients with pressure injuries, this 2025 study found self-pay patients faced the longest stays – an increase of 3.91 additional days – and incurred $21,216 more in costs compared to Medicare patients. Hispanic patients incurred $37,647 more in costs and 1.42 additional days versus White patients. Pressure injuries don’t distribute their… Read Full Article
Title
Assessment of Malpractice Claims Associated With Pressure Ulcers
Key Takeaway/s
Hospitals are named as defendants in 62% of pressure ulcer malpractice cases, with mean payouts of $1.6–$2.5 million when they lose. Nursing homes face mean awards exceeding $4 million. Negligence, not malpractice, is the primary claim in 76% of cases, meaning jurors view pressure injuries as failures of basic care, not complex medical judgment. Read Full Article
Title
Long-Term Care Liability for Pressure Ulcers
Key Takeaway/s
Plaintiffs recovered damages in 87% of pressure ulcer lawsuits with a median settlement of $1.06 million, and awards reaching as high as $312 million. More than 17,000 PI-related lawsuits are filed in the US annually – making pressure injuries the second most common cause of malpractice claims. Even facilities that believed their care was adequate… Read Full Article
Title
Pressure Ulcers: Impact on Hospital Costs and Length of Stay
Key Takeaway/s
This University of Alabama at Birmingham hospital study found that developing a hospital-acquired Stage II+ pressure ulcer was associated with substantially higher hospital costs and longer stays. Mean unadjusted costs were $37,288 vs $13,924 and LOS 30.4 vs 12.8 days. Even after adjustment, costs and LOS remained significantly higher. Read Full Article
Title
Key Takeaway/s
This UAB tertiary teaching-hospital study found that patients who developed hospital-acquired pressure ulcers incurred substantially higher costs and longer stays. Adjusted analyses showed costs of $29,048 vs $13,819 and length of stay of 20.9 vs 12.7 days, confirming pressure ulcers independently drive excess inpatient utilization beyond baseline severity. Read Full Article
Title
Hospitalizations Related to Pressure Ulcers among Adults 18 Years and Older, 2006
Key Takeaway/s
AHRQ HCUP data show pressure-ulcer–related adult hospitalizations carried materially higher utilization and cost: mean stay 12.7–14.1 days vs 5.0 days without pressure ulcers, and mean cost per stay $16,800–$20,400 vs $9,900. Over half were discharged to long-term care, and mortality was higher. Read Full Article
Title
Quality of Life of Patients with Pressure Ulcers: A Systematic Review
Key Takeaway/s
Patients with pressure injuries experience severely diminished quality of life across every dimension – physical, emotional, social, and cognitive. Pain is the defining and relentless feature, described by patients as leading to helplessness, despair, and complete dependence. Behind every statistic is a person whose life has been fundamentally diminished by a preventable wound. Read Full Article
Title
Key Takeaway/s
Among 676,435 hospitalized patients with pressure ulcers, median length of stay was 7 days versus 3 days for those without – more than double. Hospital stays involving a pressure ulcer may incur additional annual charges of up to $700,000. Patients with PIs were significantly more likely to have longer stays, higher charges, and worse outcomes… Read Full Article
Title
Visual Feedback of Continuous Bedside Pressure Mapping to Optimize Effective Patient Repositioning
Key Takeaway/s
Visual feedback from continuous bedside pressure mapping enabled caregivers to reposition patients more effectively, lowering high pressures and improving care. Read Full Article
Title
Key Takeaway/s
This UAB tertiary teaching-hospital study found that patients who developed hospital-acquired pressure ulcers incurred substantially higher costs and longer stays. Adjusted analyses showed costs of $29,048 vs $13,819 and length of stay of 20.9 vs 12.7 days, confirming pressure ulcers independently drive excess inpatient utilization beyond baseline severity. Read Full Article
Title
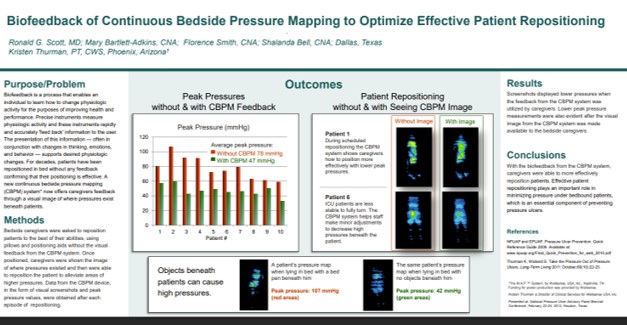
Biofeedback of Continuous Bedside Pressure Mapping to Optimize Effective Patient Repositioning
Key Takeaway/s
At a Dallas-area long-term acute care facility, real-time pressure visualization reduced average peak pressures by 40% – from 78 mmHg to 47 mmHg. 100% of caregivers reported more effective repositioning with the pressure image than without it, including for patients too medically complex to fully turn. Hidden objects beneath patients – including a bedpan producing… Read Full Article
Title
Key Takeaway/s
This peer-reviewed study found that when staff repositioned residents using feedback from a real-time pressure mapping system, peak interface pressures were significantly reduced (P = .016) and more preventive interventions were implemented (P = .012), demonstrating that pressure visualization directly improves the effectiveness of repositioning Read Full Article
Title
Reducing Pressure Ulcer Development in the ICU
Key Takeaway/s
At Henry Ford Health System’s Medical ICU (Detroit), implementing real-time pressure visualization on 20 ICU beds was associated with a ~94% reduction in institution-related pressure ulcers versus the same months the prior year (16 to 1; 5% to 0.3%). The study reported no technical or safety issues and strong caregiver acceptance. Read Full Article
Title
Key Takeaway/s
Real-time pressure mapping in ICUs, geriatric wards, operating rooms, and long-term care consistently showed that visual feedback allowed staff to identify high-risk zones, reposition more effectively, and prevent hospital-acquired pressure ulcers while also supporting wound healing. Read Full Article
Title
Key Takeaway/s
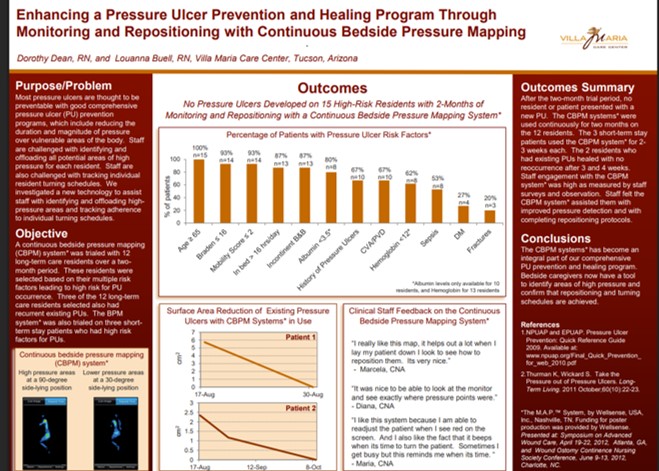
At Villa Maria Care Center, Continuous Bedside Pressure Mapping over two months prevented all new pressure ulcers in 15 high-risk residents, supported healing of existing ulcers with no recurrence, and became an integral part of the pressure ulcer prevention program. Read Full Article
Title
Key Takeaway/s
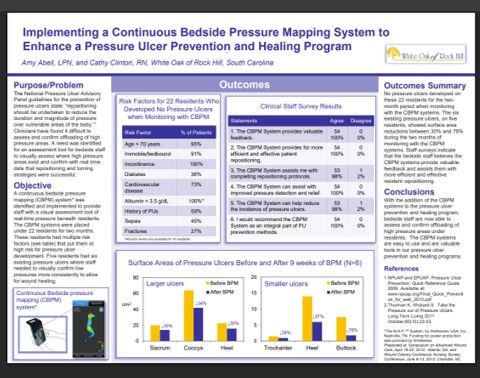
At White Oak of Rock Hill, no new pressure ulcers developed in 22 high-risk residents monitored with bedside pressure visualization, while existing ulcers showed 30–76% surface area reduction within 9 weeks Read Full Article
Title
Pressure Map Technology for Pressure Ulcer Patients: Can We Handle the Truth?
Key Takeaway/s
In a 55-bed LTAC facility in North Texas, pressure mapping technology improved nursing practice, reducing average turn delays by 63% and median delays by 56%, thereby lowering risk of tissue damage. Read Full Article
Title
Effectively Addressing Hospital-Acquired Pressure Injuries With a Multidisciplinary Approach
Key Takeaway/s
Effectively Addressing Hospital-Acquired Pressure Injuries With a Multidisciplinary Approach Read Full Article
Title
Key Takeaway/s
Overall, the annual prevalence of pressure injuries and annual mean hospitalization cost increased ($69,499.29 to $102,939.14). Read Full Article
Title
Key Takeaway/s
This 2020 national hospital database study concluded that each hospital-acquired pressure injury added about $21,767 in hospital cost per patient versus no pressure injury, equal to about $30,000 in 2026 dollars. Read Full Article
Title
Value of hospital resources for effective pressure injury prevention: a cost-effective analysis
Key Takeaway/s
This peer-reviewed BMJ Quality & Safety cost-effectiveness study analyzed 34,000+ hospital patients and quantified the financial impact of severe pressure injuries. It reported that Stage 3–4 (full-thickness) pressure injuries add about $6,209 per patient-day, underscoring the high daily cost burden and the value of effective, hospital-wide prevention. Read Full Article
Title
The national cost of hospital-acquired pressure injuries in the United States
Key Takeaway/s
This 2019 study estimated that each hospital-acquired pressure injury adds about $10,708 per patient on average (≈ $14,500 today), calculated by distributing the total national HAPI cost burden across all patients who develop a HAPI, contributing to $26.8 billion annually (≈ $36.5 billion today). Read Full Article
Title
High cost of stage IV pressure ulcers
Key Takeaway/s
This study from NYU School of Medicine found Stage IV pressure ulcers cost about $125k–$129k per patient in hospital treatment costs when ulcer-related complications were included. These costs are far higher than prior estimates and emphasize early recognition and treatment to stop progression to Stage IV and avoid extreme, non-reimbursed “never event” costs. Read Full Article
Title
Cost of Treating Pressure Ulcers for Veterans with Spinal Cord Injury
Key Takeaway/s
“In a VA study of veterans with spinal cord injury, the presence of a pressure injury increased average health care costs by $77,587 compared to those without, driven by higher inpatient costs, emphasizing the need for prevention.” Read Full Article
Title
Pressure Ulcers: Impact on Hospital Costs and Length of Stay
Key Takeaway/s
This University of Alabama at Birmingham hospital study found that developing a hospital-acquired Stage II+ pressure ulcer was associated with substantially higher hospital costs and longer stays. Mean unadjusted costs were $37,288 vs $13,924 and LOS 30.4 vs 12.8 days. Even after adjustment, costs and LOS remained significantly higher. Read Full Article
Title
Hospitalizations Related to Pressure Ulcers among Adults 18 Years and Older, 2006
Key Takeaway/s
AHRQ HCUP data show pressure-ulcer–related adult hospitalizations carried materially higher utilization and cost: mean stay 12.7–14.1 days vs 5.0 days without pressure ulcers, and mean cost per stay $16,800–$20,400 vs $9,900. Over half were discharged to long-term care, and mortality was higher. Read Full Article
Title
Key Takeaway/s
In elderly care, pressure mapping directly supported staff education by improving pressure-injury awareness, strengthening repositioning decisions with visual feedback, and increasing the frequency and appropriateness of preventative interventions during routine care. Read Full Article
Title
Pressure Map Technology for Pressure Ulcer Patients: Can We Handle the Truth?
Key Takeaway/s
Pressure mapping improved workflow performance in a long-term acute care setting by reducing delays to scheduled turning, supporting more reliable execution of turning protocols, and creating clearer accountability around when repositioning actually occurs. Read Full Article
Title
Self-turning for Pressure Injury Prevention
Key Takeaway/s
Pressure visualization can be used as a structured education tool for appropriate patients, enabling them to learn and reliably perform self-repositioning with clear visual guidance, reducing staff burden while keeping turning technique verifiable. Read Full Article
Title
Key Takeaway/s
Across multiple care settings, the evidence supports pressure visualization as a workforce enablement tool: it makes prevention practices more consistent, improves staff decision-making with real-time feedback, and strengthens training and standardization of repositioning technique. Read Full Article
Title
Self-turning for Pressure Injury Prevention
Key Takeaway/s
When appropriate patients were identified as able to self-turn, real-time pressure visualization helped them reposition themselves reliably with clear, immediate feedback. This demonstrates that pressure visualization can actively engage patients in their own pressure management, supporting safer self-directed turning when clinically appropriate. Read Full Article
Title
Key Takeaway/s
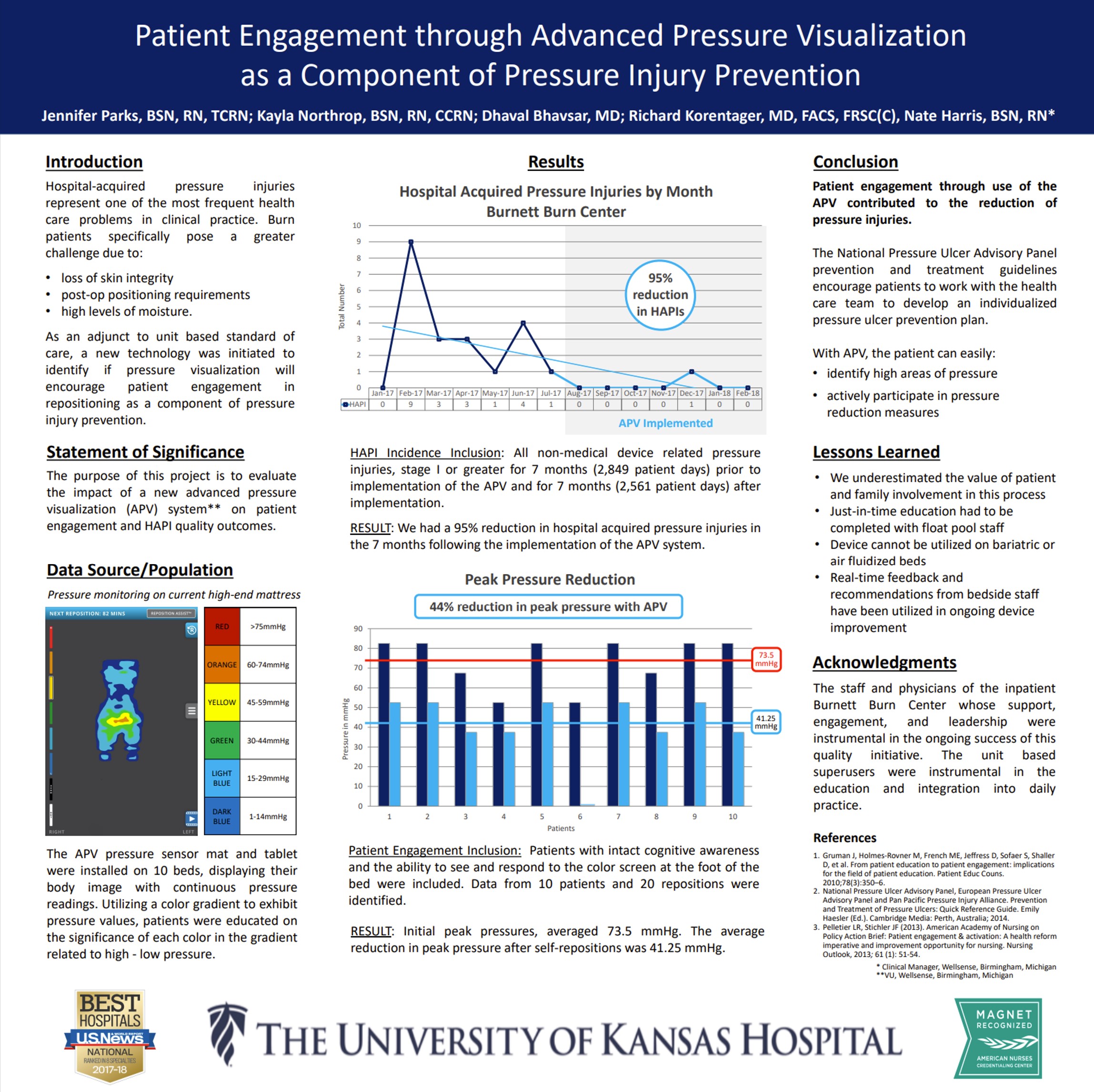
This study frames pressure visualization as a patient-facing tool: by making pressure visible, it motivates participation and supports behavior change around repositioning. The work reinforces that engagement improves when patients can see the cause-and-effect of their own movement on pressure. Read Full Article
Title
Key Takeaway/s
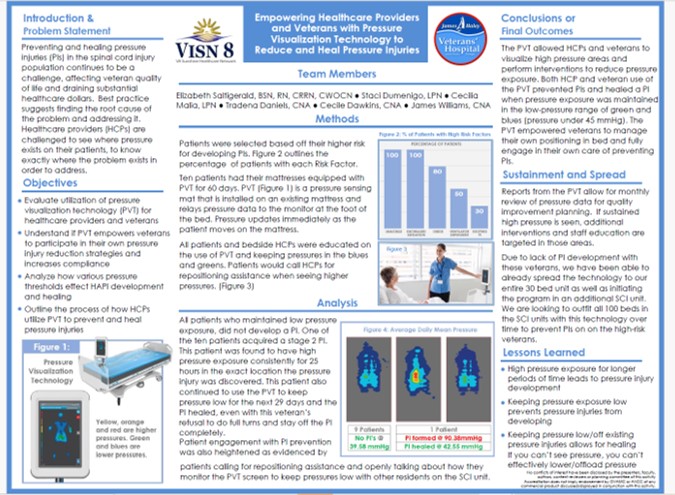
In a veteran population, pressure visualization was used not only to guide clinical care but to empower patients and caregivers with understandable, visual information about pressure risk. This supports greater patient involvement in day-to-day positioning decisions and reinforces shared accountability for prevention and healing. Read Full Article
Title
Key Takeaway/s
In two acute orthopedic trauma wards, patients and families reported the pressure visualization system was helpful, indicating strong engagement with the care process. The findings suggest that making pressure visible can improve patient and family understanding of repositioning goals and increase participation in prevention efforts. Read Full Article