Select a category to explore
Title
High cost of stage IV pressure ulcers
Key Takeaway/s
This study from NYU School of Medicine found Stage IV pressure ulcers cost about $125k–$129k per patient in hospital treatment costs when ulcer-related complications were included. These costs are far higher than prior estimates and emphasize early recognition and treatment to stop progression to Stage IV and avoid extreme, non-reimbursed “never event” costs. Read Full Article
Title
Key Takeaway/s
Analyzing 1.25 million US patients with pressure injuries, this 2025 study found self-pay patients faced the longest stays – an increase of 3.91 additional days – and incurred $21,216 more in costs compared to Medicare patients. Hispanic patients incurred $37,647 more in costs and 1.42 additional days versus White patients. Pressure injuries don’t distribute their… Read Full Article
Title
Assessment of Malpractice Claims Associated With Pressure Ulcers
Key Takeaway/s
Hospitals are named as defendants in 62% of pressure ulcer malpractice cases, with mean payouts of $1.6–$2.5 million when they lose. Nursing homes face mean awards exceeding $4 million. Negligence, not malpractice, is the primary claim in 76% of cases, meaning jurors view pressure injuries as failures of basic care, not complex medical judgment. Read Full Article
Title
Long-Term Care Liability for Pressure Ulcers
Key Takeaway/s
Plaintiffs recovered damages in 87% of pressure ulcer lawsuits with a median settlement of $1.06 million, and awards reaching as high as $312 million. More than 17,000 PI-related lawsuits are filed in the US annually – making pressure injuries the second most common cause of malpractice claims. Even facilities that believed their care was adequate… Read Full Article
Title
Pressure Ulcers: Impact on Hospital Costs and Length of Stay
Key Takeaway/s
This University of Alabama at Birmingham hospital study found that developing a hospital-acquired Stage II+ pressure ulcer was associated with substantially higher hospital costs and longer stays. Mean unadjusted costs were $37,288 vs $13,924 and LOS 30.4 vs 12.8 days. Even after adjustment, costs and LOS remained significantly higher. Read Full Article
Title
Key Takeaway/s
This UAB tertiary teaching-hospital study found that patients who developed hospital-acquired pressure ulcers incurred substantially higher costs and longer stays. Adjusted analyses showed costs of $29,048 vs $13,819 and length of stay of 20.9 vs 12.7 days, confirming pressure ulcers independently drive excess inpatient utilization beyond baseline severity. Read Full Article
Title
Hospitalizations Related to Pressure Ulcers among Adults 18 Years and Older, 2006
Key Takeaway/s
AHRQ HCUP data show pressure-ulcer–related adult hospitalizations carried materially higher utilization and cost: mean stay 12.7–14.1 days vs 5.0 days without pressure ulcers, and mean cost per stay $16,800–$20,400 vs $9,900. Over half were discharged to long-term care, and mortality was higher. Read Full Article
Title
Quality of Life of Patients with Pressure Ulcers: A Systematic Review
Key Takeaway/s
Patients with pressure injuries experience severely diminished quality of life across every dimension – physical, emotional, social, and cognitive. Pain is the defining and relentless feature, described by patients as leading to helplessness, despair, and complete dependence. Behind every statistic is a person whose life has been fundamentally diminished by a preventable wound. Read Full Article
Title
Key Takeaway/s
Among 676,435 hospitalized patients with pressure ulcers, median length of stay was 7 days versus 3 days for those without – more than double. Hospital stays involving a pressure ulcer may incur additional annual charges of up to $700,000. Patients with PIs were significantly more likely to have longer stays, higher charges, and worse outcomes… Read Full Article
Title
Key Takeaway/s
In the medical ICU at Henry Ford Hospital, use of a continuous bedside pressure mapping system reduced hospital-associated pressure ulcer incidence by 81% compared to standard care, confirming that real-time visual feedback enables more effective repositioning and prevention Read Full Article
Title
Key Takeaway/s
At Swedish Medical Center, Continuous Bedside Pressure Monitoring revealed issues such as bottoming out, over-inflation, and improper default settings, and guided mattress adjustments that reduced peak pressures by up to 76%. Read Full Article
Title
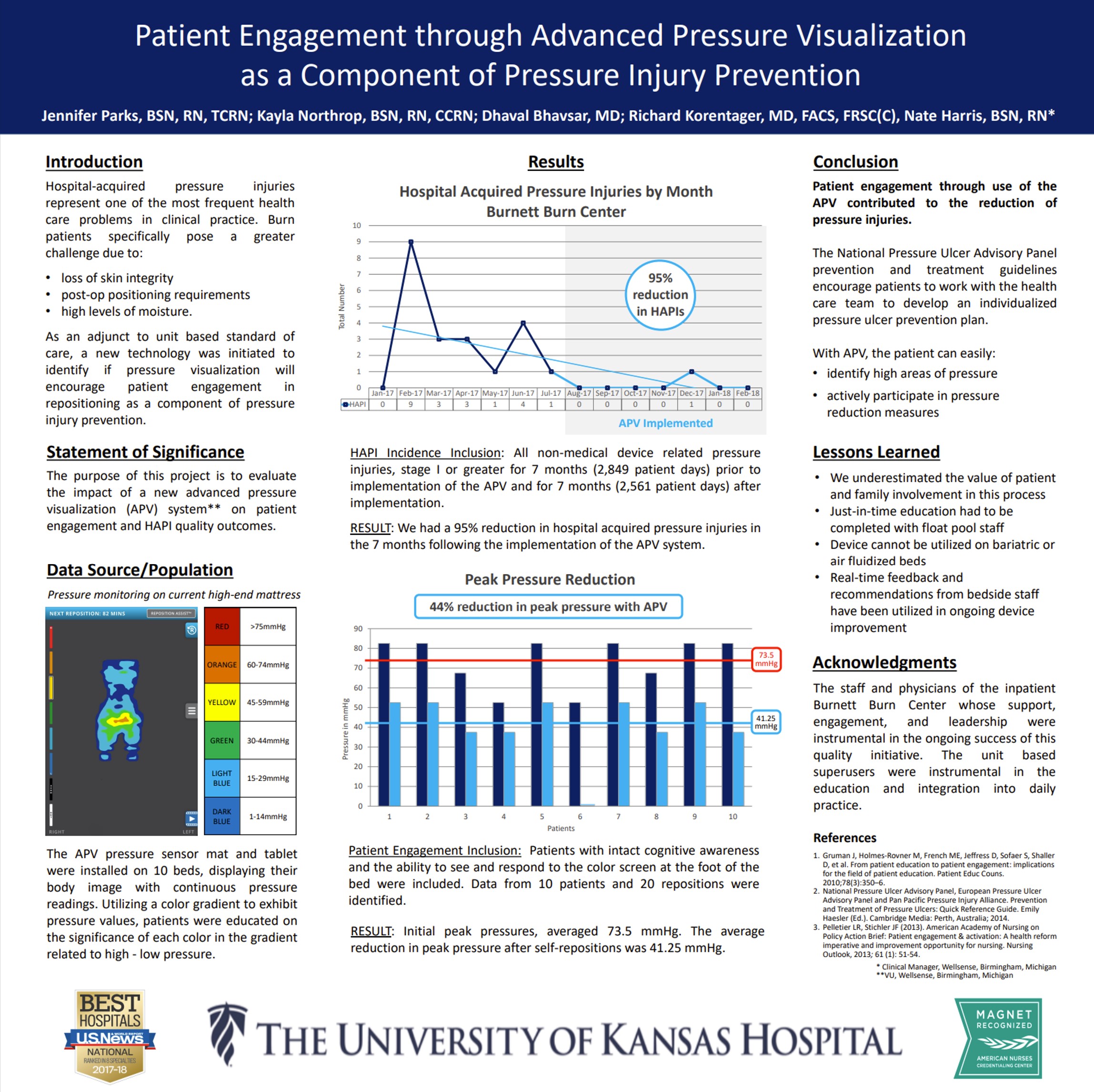
Real-Time Pressure Visualization Guides Repositioning to Reduce Hospital-Acquired Pressure Injuries
Key Takeaway/s
This real-world clinical poster from Floyd Medical Center shows that using a real-time pressure visualization monitor led to a 71% reduction in hospital-acquired pressure injuries (HAPIs) over 5 months in the critical care unit, by guiding staff to reposition patients more effectively and reduce peak pressure exposures. Read Full Article
Title
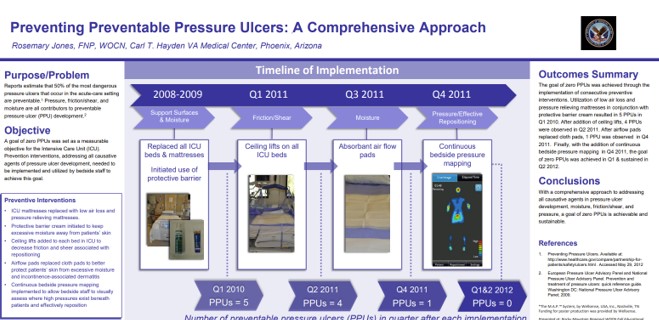
Preventing Preventable Pressure Ulcers: A Comprehensive Approach
Key Takeaway/s
At the Carl T. Hayden VA Medical Center, a stepwise prevention program that included real-time pressure visualization reduced preventable pressure ulcers (PPUs) from 5 per quarter to 0, maintaining 0 PPUs across 2 consecutive quarters. Read Full Article
Title
Self-turning for Pressure Injury Prevention
Key Takeaway/s
At Henry Ford Hospital, 101 patients identified as able to self-turn were able to reposition themselves reliably when provided a pressure-visualization system and appropriate instruction, demonstrating that mobile, lower-risk patients can self-manage turning effectively under guided use. Read Full Article
Title
Key Takeaway/s
In two UK NHS hospitals, continuous bedside pressure mapping helped identify and reduce pressure ulcer incidence, with staff reporting 100% agreement that the system improved positioning, reduced risk, and was beneficial in care. Patients and families also responded positively, with 78% rating the system helpful. Read Full Article
Title
Key Takeaway/s
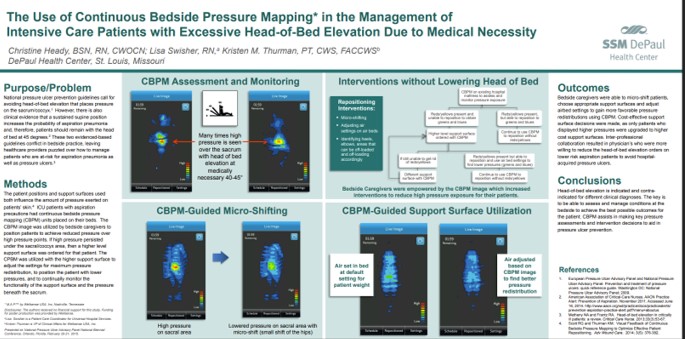
SSM DePaul Health Center showed that continuous bedside pressure mapping identified dangerously high sacral pressures at 40–45° head-of-bed elevation, enabled simple micro-shifts to reduce pressure, and guided use of higher support surfaces only when truly needed—improving outcomes and lowering costs Read Full Article
Title
Confirming Effective Off-Loading and Repositioning Using Continuous Bedside Pressure Mapping
Key Takeaway/s
A study at Swedish Medical Center found that Continuous Bedside Pressure Mapping confirmed effective off-loading and repositioning, consistently lowered peak pressures by up to 55%, and identified hidden objects such as phones and tape rolls that created high pressure beneath patients. Read Full Article
Title
Key Takeaway/s
Real-time pressure visualization significantly reduced peak interface pressures and increased both patient comfort and the number of pressure-reducing interventions performed by nurses. Staff found the system easy to use and viewed it as a valuable tool for improving repositioning technique. Read Full Article
Title
Key Takeaway/s
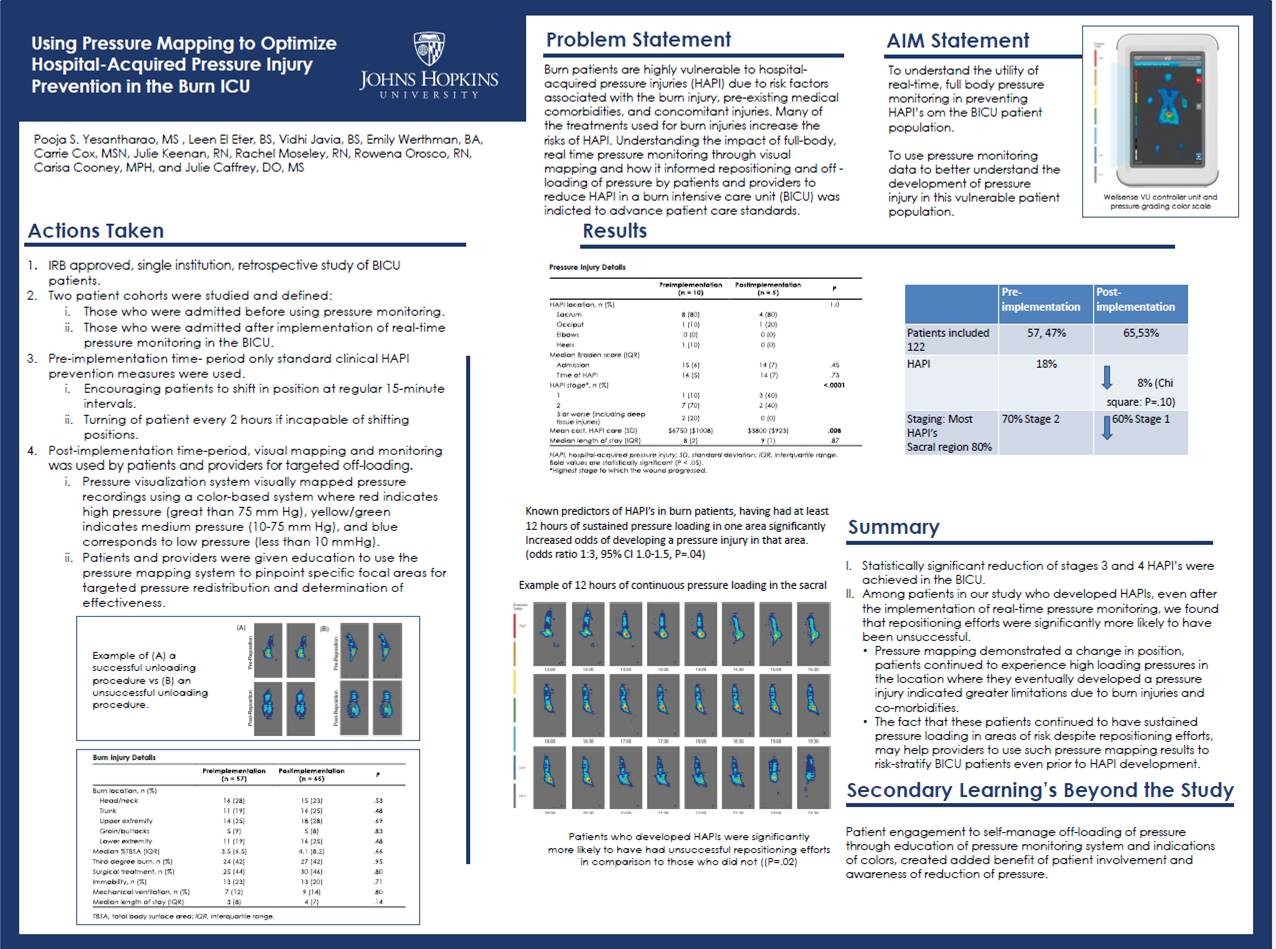
This Hopkins burn ICU study found that implementing real-time pressure mapping reduced HAPI-related care costs from about $6,750 to $3,800 per patient. These savings reflect direct pressure-injury treatment costs only (e.g., wound care), not systemic complications or extended hospitalization, and were driven by fewer and less severe pressure injuries Read Full Article
Title
Key Takeaway/s
At St. Anthony’s Medical Center, Continuous Bedside Pressure Mapping enabled use of lower-cost support surfaces, reducing reliance on specialty rentals and delivering net savings of $19 per patient per day after including the cost of the visualization system itself. Read Full Article
Title
Pressure Mapping: A New Path to Pressure-Ulcer Prevention
Key Takeaway/s
Pressure mapping gives clinicians immediate visual feedback on where pressure remains, turning “best-practice” repositioning into a teachable, repeatable workflow. It helps staff validate that a turn or support-surface change actually relieved pressure, rather than relying on skin checks, habit, or patient report. Read Full Article
Title
Key Takeaway/s
Real-time pressure feedback accelerates skills training by showing student nurses, instantly, whether a positioning change actually reduces interface pressure. This turns pressure-injury prevention from a theoretical lesson into a measurable competency and supports more consistent technique across learners and instructors. Read Full Article
Title
The wound/burn guidelines – 2: Guidelines for the diagnosis and treatment for pressure ulcers
Key Takeaway/s
These guidelines reinforce a workflow principle: repositioning should be verified with objective interface pressure measurement. They direct caregivers to check sacral pressure with an interface pressure meter, moving practice from routine turning to measured confirmation. Read Full Article
Title
Key Takeaway/s
Continuous bedside pressure mapping functioned as a real-time “quality control” layer for staff by quickly exposing common setup and support-surface errors (eg, bottoming out, over-inflation, incorrect default settings) and guiding corrective actions at the bedside. Read Full Article
Title
Confirming Effective Off-Loading and Repositioning Using Continuous Bedside Pressure Mapping
Key Takeaway/s
Pressure mapping strengthened bedside workflow by allowing staff to visually confirm that a turn actually offloaded pressure, and by helping staff identify and remove hidden causes of high pressure (workflow-relevant problems that are easy to miss during routine care). Read Full Article
Title
Key Takeaway/s
When clinical requirements force elevated head-of-bed, pressure mapping supports safer, repeatable micro-adjustment workflows by showing staff when sacral pressures become excessive and guiding small positioning changes that meaningfully reduce pressure without disrupting the care plan. Read Full Article
Title
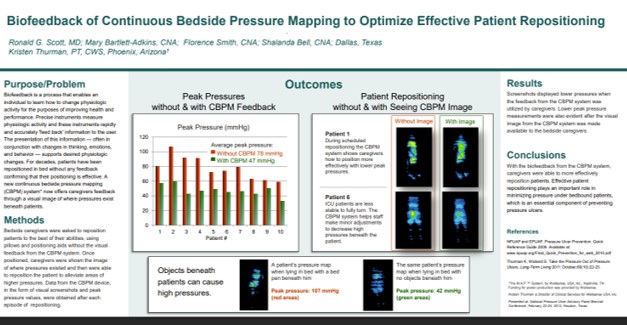
Biofeedback of Continuous Bedside Pressure Mapping to Optimize Effective Patient Repositioning
Key Takeaway/s
This work highlights the training and technique benefit of biofeedback: staff can use live pressure visualization to refine repositioning in real time and standardize “what good looks like,” improving consistency of technique across caregivers. Read Full Article
Title
Visual Feedback of Continuous Bedside Pressure Mapping to Optimize Effective Patient Repositioning
Key Takeaway/s
Visual pressure feedback improves day-to-day nursing workflow by making repositioning more teachable and repeatable, helping caregivers quickly identify high-pressure areas and adjust positioning until pressure reduction is confirmed. Read Full Article
Title
Key Takeaway/s
Real-time interface-pressure feedback supports better bedside practice by helping nurses identify effective repositioning targets, increasing pressure-reducing interventions, and reinforcing technique through immediate confirmation rather than assumption. Read Full Article
Title
Self-turning for Pressure Injury Prevention
Key Takeaway/s
When appropriate patients were identified as able to self-turn, real-time pressure visualization helped them reposition themselves reliably with clear, immediate feedback. This demonstrates that pressure visualization can actively engage patients in their own pressure management, supporting safer self-directed turning when clinically appropriate. Read Full Article
Title
Key Takeaway/s
This study frames pressure visualization as a patient-facing tool: by making pressure visible, it motivates participation and supports behavior change around repositioning. The work reinforces that engagement improves when patients can see the cause-and-effect of their own movement on pressure. Read Full Article
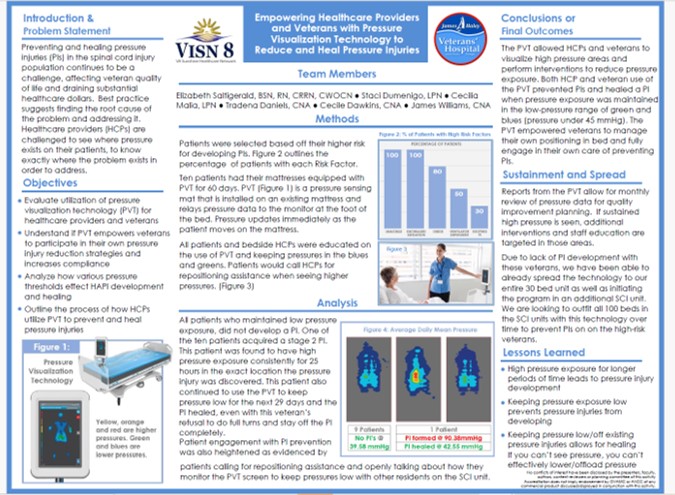
Title
Key Takeaway/s
In a veteran population, pressure visualization was used not only to guide clinical care but to empower patients and caregivers with understandable, visual information about pressure risk. This supports greater patient involvement in day-to-day positioning decisions and reinforces shared accountability for prevention and healing. Read Full Article
Title
Key Takeaway/s
In two acute orthopedic trauma wards, patients and families reported the pressure visualization system was helpful, indicating strong engagement with the care process. The findings suggest that making pressure visible can improve patient and family understanding of repositioning goals and increase participation in prevention efforts. Read Full Article